Menu
Achieve 20|20 vision with UK’s leading laser eye surgeon and free yourself from the hassle of contact lenses or glasses. Book a consultation today & take the next step towards better vision.


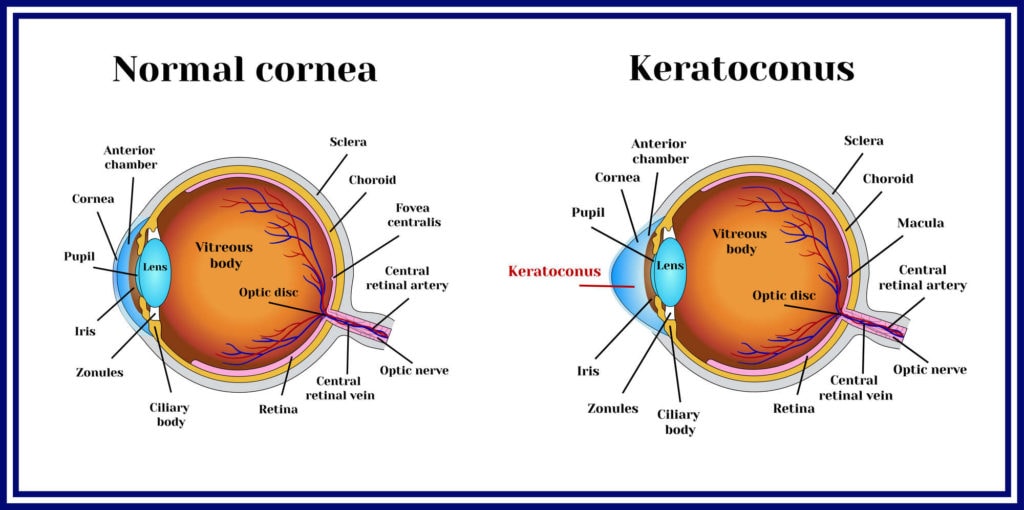
Keratoconus (KCS) is a degenerative condition of the cornea which may have an inherited component. It affects around 1 in 1500 people in the UK but the incidence can be as high as 1 in 450 people in some populations. The disease process is one of corneal thinning called ectasia, which usually starts in teenage years and stabilizes in the late 20’s to 30’s but can be highly variable. Keratoconus is often associated with allergic conditions such as eczema, asthma or hay fever and is made worse by eye rubbing.
The cornea is the transparent dome of collagenous tissue that forms the front protective coat of the eye. It is very nearly round in shape and is responsible for about two thirds of the optical power, or focusing power of the eye. Thinning of the cornea causes it to lose its natural curvature and bow out of shape, this irregular astigmatism results in light being focused in many different directions which causes blur and reduced visual quality.
At night our pupils get bigger so that our eyes can use all available light to see. As the cornea in KCS is irregular, more poorly focused light enters a larger pupil leading to increased light scatter which is perceived as glare or starburst and visual quality falls further. This can cause particular problems e.g. driving at night.
Patients will often be aware that they cannot see as sharply as they are used to, particularly when using screens but because KCS typically affects one eye much more than the other, the overall vision may remain quite good and diagnosis of KCS is often made late because routine sight tests may not be requested. Opticians are good at detecting KCS because they notice abnormal reflexes when examining the eye, these are described as ‘oil drop’ or ‘scissoring’. They will also measure astigmatism and will expect to correct vision fully in both eyes so the presence of high astigmatism, changing astigmatism or reduced vision will prompt referral.
There are two main aims of treatment:
These treatments may be combined or performed separately, therapeutic treatment is always the first priority.
Keratoconus causes complex changes in the visual system and treatment is highly individual, particularly when improving vision because each treatment protocol is customized for the eye of that particular patient. If you don’t find the answers you’re looking for, please get in touch – we are happy to help.
Corneal collagen cross-linkage (CXL) is the first and most effective treatment shown to stabilise KCS, it was developed in Switzerland in the late 90’s and was approved by NICE in the UK in 2009. It has been extensively investigated and epi-off CXL is considered the gold standard in treatment.
David Anderson has been performing CXL since 2010 and uses the Avedro KXL system which is considered to be the most advanced platform for treating KCS with more than 400,000 treatments to date.
Think of the cornea as a transparent rubber ball anchored around the edge where it meets the white part of the eye (the sclera). Bending or stretching the cornea in one direction causes an equal change in the opposite direction. Using the Visumax laser to create a tiny channel in the cornea 1mm in width, thin plastic semi-circular intra-corneal ring segments (ICR’s) are painlessly inserted into the channel to flatten the steeper parts of the cornea and steepen the flatter making the overall shape rounder.
Trans-epithelial phototherapeutic keratectomy (PTK) is a surface laser procedure using the Mel90 excimer laser designed to remove a very small amount of tissue immediately prior to CXL. As the cornea in KCS is steeper and more irregular in shape than normal, the use of a regular beam profile can help smooth the cornea a little at the same time that CXL is performed. As the corneal epithelium needs to be removed for each procedure individually, combining the two, reducing healing time.
Topography-guided photorefractive keratectomy (Topo-PRK) is an excimer laser treatment designed to reshape the cornea to a rounder or more natural shape and reduce the distortion caused by KCS. Detailed measurements are made of the cornea using two different specialist non-contact measurement devices, the Pentacam HR and the CRS-Master. From these readings the corneal shape can be analysed and a custom treatment designed for that individual cornea and applied using advanced surface ablation.
Implantable collamer lens surgery (ICL) is a surgery that can be used either as a primary measure to improve vision in KCS in stable disease or following CXL or other refractive treatments designed to reduce irregular astigmatism e.g. ICR surgery or topo-PRK.
ICL surgery is covered more completely in another section of the website, please find the link here.
Nuffield Health Wessex Hospital
Winchester Road, Chandlers Ford
Eastleigh, Hampshire
SO53 2DW
© Anderson Eye Care 2020. All Rights Reserved. Made by Digital Roo.
Enter your details below to get instant access to your free laser eye surgery infopack.